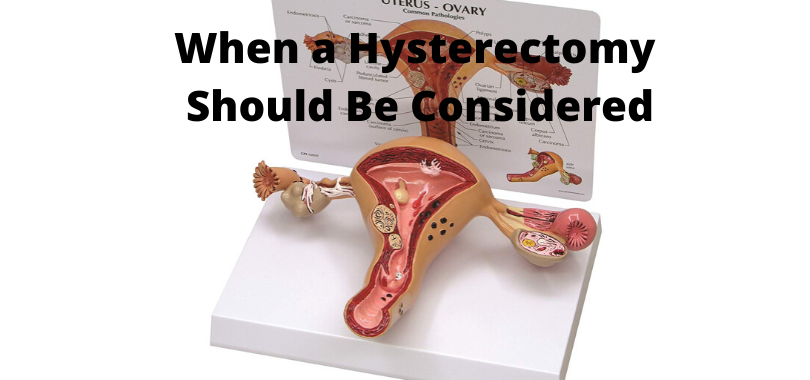
One of the most common questions that I get asked from women with endometriosis is “Is there a link between endometriosis and cancer?”
There has been many research papers on this and there is some evidence to suggest that women with endometriosis may have a higher risk of certain cancers such as endometrial cancer and also ovarian cancer.
We all know that Endometriosis is a debilitating disease, but many people don’t realise the possible future implications of this disease, mixed with our highly inflammatory diets and lifestyle. Unfortunately it is a recipe for any inflammatory disease, and for expression of cancer cells.
There have been many reputable studies to date showing the link between inflammation and cancer and endometriosis is definitely an inflammatory disease that needs proper management otherwise some studies are now suggesting it could be a precursor to certain cancers.
This isn’t meant to scare anyone either. It is just to help people realise the possible implications of this disease and to be more proactive around getting yourself and your body healthier and also being properly managed by a qualified health professional. When it come to cancerous states, prevention is key and early intervention is also.
Better education is needed
Given that, we need to really take this disease more seriously than many people with the disease and many in the medical community probably realise. Prevention is always the key to any disease and even though endometriosis cannot be prevented, early intervention and ongoing management of the disease is crucial. This is why I think all young girls should be educated about what a proper menstrual cycle should be like and that period pain is not normal. There also needs to be proper education about diet and lifestyle interventions with inflammatory diseases, such as endometriosis, and how it also needs a multimodality approach to be managed properly.
Endometriosis is like cancer in many ways
Endometriosis, like cancer, is characterised by cell invasion and unrestrained growth. Furthermore, endometriosis and cancer are similar in other aspects, such as the development of new blood vessels and a decrease in the number of cells undergoing apoptosis. In spite of these similarities, endometriosis is not considered a malignant disorder.
The possibility that endometriosis could, however, transform and become cancer has been debated in the literature since 1925. Mutations in the certain genes have been implicated in the cause of endometriosis and in the progression to cancer of the ovary (Swiersz 2006). There is also data to support that ovarian endometriosis could have the potential for malignant transformation. Epidemiologic and genetic studies support this notion. It seems that endometriosis is associated with specific types of ovarian cancer (endometrioid and clear cell) (Vlahos et al, 2010). The relationship between endometriosis and ovarian cancer is an intriguing and still poorly investigated issue. Specifically, histological findings indicate a definitive association between endometriosis and endometrioid/clear cell carcinoma of the ovary (Parihar & Mirge 2009).
Women with endometriosis may be more prone to certain cancers
There are recent studies which have shown that mutations in the certain genes found were identified in 20% of endometrial carcinomas and 20.6% of solitary endometrial cysts, played a part in the development of ovarian cancers. In addition to cancerous transformation at the site of endometriosis, there is recent evidence to indicate that having endometriosis itself may increase a woman’s risk of developing non-Hodgkin’s lymphoma, malignant melanoma, and breast cancer (Swiersz 2014).
Women with endometriosis appear to be more likely to develop certain types of cancer. Brinton, PhD, Chief of the Hormonal and Reproductive Epidemiology branch at the National Cancer Institute has studied the long-term effects of endometriosis, which led her to Sweden about 20 years ago. Using the country’s national inpatient register, she identified more than 20,000 women who had been hospitalised for endometriosis.
After an average follow-up of more than 11 years, the risk for cancer among these women was elevated by 90% for ovarian cancer, 40% for hematopoietic cancer (primarily non-Hodgkin’s lymphoma), and 30% for breast cancer. Having a longer history of endometriosis and being diagnosed at a young age were both associated with increased ovarian cancer risk (Brinton et al, 1997).
Farr Nezhat, MD, Chief of Gynecologic Minimally Invasive Surgery and Robotics at St. Luke’s and Roosevelt Hospitals in New York City and Professor of Obstetrics and Gynecology at Columbia University, spoke on the pathogenesis of endometriosis and ovarian cancer. According to a 2000 study of women with ovarian cancer by Hiroyuki Yoshikawa and colleagues, endometriosis was present in 39% of the women with clear cell tumours and 21% of those with endometrial tumours. The studies clearly suggest that Endometriosis may be the precursor of clear cell, or endometrial ovarian cancer (Yoshikawa et al, 2000).
Inflammation and Estrogens are a big factor in many cancers
If you combine inflammation with oestrogen as with both endometriosis and ovarian or uterine cancers, it’s going to be a vicious circle, as the 2 diseases share numerous other characteristics. For example, both are related to early menstrual cycles and late menopause, infertility, and inability to fall pregnant. Any factors that relieve or offer protection against both conditions need to be explored, including dietary and lifestyle changes etc.
Some authors also suggest that there is an also increased risks of colon cancer, ovarian cancer, thyroid cancer non-Hodgkin’s lymphoma and malignant melanoma in women with endometriosis when compared with the general population (Brinton et al, 2005).
Proper management and early intervention is crucial
If you do have patients with endometriosis you do need to take into consideration the future implications of this disease, not only the pain and turmoil it causes on the way, but also the future possibility that endometriosis could also lead to cervical cancer, ovarian cancer, or many of the other cancers that can be found in the body.
There are certain medications, both natural based and medical that can great assist in the treatments and management of endometriosis and microscopic endometriosis implants. These do need to be explored and we now have the Royal College of Obstetricians and Gynaecologists recommending diet and lifestyle changes and to use complementary medicine such and Chinese Herbal Medicine and Acupuncture for the the management and treatment of endometriosis. This is recommended alongside medical interventions and it does get back to a multimodality approach is the key factor in proper management of this disease.
Diet and lifestyle changes are crucial in cancer prevention
There have been numerous studies showing the benefits of a low inflammatory based diet and reduction in lifestyle factors such as stress. These things are also crucial in any inflammatory disease and certainly in cancer prevention.
Anyone with endometriosis does need to be following anti-inflammatory diet, with reduced refined foods and increased whole foods. This is something I promote whole-heartedly and see great results with on a daily basis. It is also part of my PACE- Diet and Lifestyle program. PACE meaning (Paleo/Primal Ancestral Clean Eating) .
This style of diet is very much like the mediterranean diet which is now shown to be one of the best diets in the world to help with cancer prevention and reduction of cardiovascular disease. It is something that has been shown to assist with inflammatory diseases such as endometriosis. This can be done alongside supplements such as omega 3 oils and antioxidants that also offer protection and prevention against inflammatory diseases too. You should also talk to a qualified healthcare professional about diet and lifestyle interventions and supplementation.
See an Endometriosis Expert
Hope that helps everyone to understand why it is so important to really make some proactive changes if you do have endometriosis. You really need to explore as many options as you can when trying to manage this disease and halt its progression. It is also important to see an endometriosis expert and not try and manage this disease yourself. You just should not be doing this and it is not effective management. Always see an appropriately trained healthcare professional who is trained in endometriosis and other disease states in women. We don’t want to see it end up as cancer later on and this is why it is so important to make sure you are being appropriately managed now.
Final Word
If you do need help with endometriosis, and the associated symptoms of endometriosis, give my friendly staff a call and find out how I can help you. Always remember that early intervention is the key and being managed properly is also crucial.
Take care
Regards
Andrew Orr
-No Stone Left Unturned
-Master of Reproductive Medicine
-Master of Women’s Health Medicine
-The Endometriosis Experts